VETERINARY CLINIC - N0TE BOOK
The latest news and information from the veterinary world
to help you keep your horse a happy, healthy horse.
* * * * * *
Please note that the information contained here is to give general advice and is not necessarily specific for individual cases. You should always seek professional assistance from a veterinary surgeon if in any doubt about the condition of your horse.
 |
|
SURGERY - The Risks of Anaesthesia
Surgery on horses these days is so common people almost talk about it in a somewhat blase manner, but it is still a very risky business.
Putting aside the actual risks that are present throughout the operation, there are those encountered when a horse is coming round + all the post-operative ones too.
When a horse is recovering from anaesthesia he is placed in a padded box (or even in water) but he can still do tremendous damage to himself particularly following delicate surgery (such as colic). RODOCK is one such horse; he to be put down as a result of injury sustained following a succesful operation. How can it be that a horse can come through a possibly life-saving operation and then have to be destroyed anyway?
Unfortunately horses can injury themselves when coming around because, like us, they can have varying reactions; some take it all in their stride and although attempting to rise "realise" that all is not quite as it should be a wait a while longer before having another go - a bit like a foal trying to find its feet for the first time; sadly though, others can react quite violently in their desperate attempts to gain control of their legs again and will thrash about, getting up, stagger about and then fall down. During this sort of behaviour the horse is a great risk of damaging itself and it is especially worrying if the horse has just had an operation to a leg. This was everyone's great concern with MIA (See Mia's Story in the VET CLINIC) when she had some of her cannon bone scrapped away - an already weakened bone was particularly vulnerable to the added trauma.
Although not statistically recognised as being a hard fact, it would seem that horses that undergo an operation because of an illness, such as colic, so are depressed and subdued anyway, are less prone to violent outbursts compared to those that are effectively physically fit but have to undergo either unexpected surgery (say, because of a riding accident) or for routine treatment (such as castration) so have not necessarily be let down, switched off and rested.
Of course problems can also set in even if a horse appears to have made a seemingly good recovery from his operational ordeal. Bannow Bay underwent routine surgery to remove a floating bone chip from his knee. The operation itself went well but the horse apparently appeared a little depressed (which is only really to be expected), but overnight there was a little blood from his nose. Investigation upon being taken to veterinary surgeons revealed a serious situation, possible haemorrhaging and there was no alternative but to put Bannow Bay down.
Then of course the actual operation itself is a risk. Horses are known to be high-risk patients with 2% having life-threatening reactions to the drugs used, the very postion in which a horse lays can cause problems, blood-pressure fluctuations, there is quite a list, but as an owner you should be made aware of these.
So if your horse should need to undergo surgery make sure you discuss fully all the implications with your vet beforehand.
Also you should read the article entitled "Equine Anaesthesia" in the VET CLINIC for more in-depth information about equine surgery.
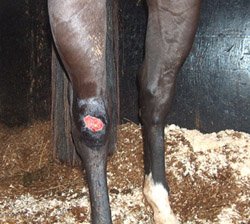
MUD FEVER
The return of the wet weather has once again produced mud fever in quite a large number of horses and ponies around the country.
The reason why mud fever is only prevalent in the winter months is because it is a bacteria (dermatophilus congolensis ) which lies dormant in the ground throughout the drier summer months, emerging in its best-loved conditions - wet and mild (as opposed to frosty) – just what we are experiencing again at present.
Usually horses that are generally healthy can resist attack but with the constant wet and muddy conditions the more sensitive skin of the heel region becomes softened and consequently vulnerable to chafing and/or chapping from the constant rain and mud (you know yourself how your skins changes if you have had your hands in water for any length of time, or in colder weather how easy it is for your hands to become sore if they keep getting wet); only the slightest crack in the skin is enough for the tiny anaerobic bacteria to penetrate. Any areas of cuts or abrasions are also vulnerable.
You'll soon detect whether your horse has fallen victim to mud fever because your attention will be drawn to matted hair around the heels, base of the fetlocks and pasterns; in more severe cases it can spread up the back of the tendons and even to the underside of the torso (if the back is affected the condition is termed rain scald). Closer examination will reveal crusty scabs which weep a yellowy serum; the surrounding skin will probably be red; inflammation may or may not be present. Lameness will be evident in the more severe cases because of the infection and resultant inflammation so there will be heat in the legs.
Even mild infections can be stubborn to clear up and diligent attention is required.
What to do
In mild cases wash the infected area (we recommend HIBISCRUB) and thoroughly dry the skin. Apply a anti-bacterial cream such as PROTOCON OINTMENT.
In cases were the infection is more severe, do not be tempted to pick and pull at the scabs as not only will this be painful, it will also encourage further infection; instead apply an emollient cream (such as UDDER CREAM) which will gently and naturally soften the skin and loosen the scabs (thus also providing relief), as well as making the skin less prone to cracking open because it is once again pliant. Then apply an antibiotic/anti-inflammatory/anti-fungal ointment. Keep the legs clean and dry with gamgee under bandages, but remove these reguarly and allow the skin to breathe which will aid healing.
If your horse has a very severe infection to the point that he is evidently in some discomfort then you should call your vet to administer antibiotics.
It is preferable to keep your horse stabled until any infection had cleared but this is not always possible so apply plenty of barrier cream before turning out.
How can you prevent or reduce the risk of mud fever?
1) The only way is to keep a horse's legs as clean and dry as possible so do not be tempted to keep washing off mud, etc. Instead let it dry and then brush it off. If you do choose the washing option, then do not hot water as this more readily softens the skin making it more vulnerable – so uncomfortable as it may be for you – use just tepid water. ALWAYS dry the legs thoroughly after any washing or if your horse comes in with wet legs.
2) Apply a barrier cream to the heels of turned out horses.
3) Don't be tempted to trim away too much of the natural feather; granted, the long hair helps harbour the infection, lack of it has the opposite effect as it is actually natural protection, the long hair acting as "a water run-off system". So reduce the length but do not clip the heels right out.
4) Reduce the amount of turn out time you allow your horse during prolonged wet periods.
5) Some pasture harbours the bacteria more readily than others so is "permanently infected". Only by experimenting will you establish if yours is such a one.
6) Keep the insides of boots and rugs as clean as possible.
7) Check that these items are not causing damage to the skin thus giving the mud fever bacteria a ready-made access point.
8) Make sure that you are not using any disinfectants/bedding/medication that is irritations or allergic reactions.
9) Remember that white legged/heavily feathered horses, youngsters and horses not in the best of condition are more susceptible to mud fever.
VACCINE REACTIONS
Although extremely rare, it does happen - a reaction to an injected vaccine.
As owners we tend to readily and routinely (and quite rightly so) have our horses vaccinated against flu, tetanus and so on. Advances in veterinary science have meant that in all but a few cases, a given vaccination could indeed be a life saving one. However, what happens in cases where there is an adverse reaction?
Despite the rarity of such occurrence, owners should discuss the matter with their veterinary surgeon so that they are aware of the implications and, of course, so that vets do not "play god" anymore than a considerable number of them try to do. As every boy scout will tell you, you should be prepared - your horse might just turn out to be one of those rare cases.
A mild reaction to a vaccine is reasonably common i.e. the stiff neck syndrone where by the horse is visibly stiff in its neck for a few days after a jab. This is why you should avoid having vaccinations a couple of days before attending a show. Sometimes the muscle surrounding where the needle was inserted actually goes hard and, sometimes, lumpy in which case you should apply cold packs. If the hardness does not subside after a few days, then the application of hot packs will help ease the tension.
As we know ourselves, sometimes after a vaccination we can not feel uite 100& for a day or so, and this is equally applicable to your horse; he can become a little depressed and his appetite can drop for a couple of days. In such instance, the most important management aspect is to keep an eye on your horse's temperature. An increase up to 105 is not unusual but should it increase above this then your should call your vet. Likewise be aware that heart and respiration rates can also go up and, again, you should call your vet, as you should also do if the depression/suppressed appetite continues for more than 48 hours.
In a more serious case an abscess can actually form on the neck and whilst they more often than not are a sterile inflammatory reaction to the vaccine, they can also be the result of an infection rather than the vaccine. In these cases the cause is due to a foreign body or contaminant of some sort being on the skin as the needle punctures it. In either situation a vet may be required to lance the abscess as they do not always burst of their own accord. A horse with an abscess should be closely monitored for adverse signs - loss of appetite, depression, increased heart/respiration rates and so on. Infections, as we know ourselves, can make us feel pretty rotten.
Certain types of bacteria produce a gas which collects under the skin forming an air pocket, so if when you touch the horse's skin you hear a crackling sort of sound, then this is what has happened and you need your vet immediately, especially if your horse is exhibiting any other negative health signs.
The most severe reactions (which are no more likely than your horse being struck by lightning) are when horses actually have allergic reactions. This is known as ANALPHYLACTIC SHOCK.
This is extremely serious and dangerous - horses die if they do not receive immediate veterinary attention. This is why, strictly, a vet should remain in the yard for 15-20 minutes after a vaccine has been adminstered - just in case!! Blood pressure drops dramatically and fluid rapidly accumulates in the lungs which is fatal if drugs are not given to boost the heart rate and pump the blood pressure back up.
This information is not intended to put owners off having their routine vaccinations as undoubtedly these have prevented countless deaths from all many of diseases that threaten horses' lives. It is only intended to raise awareness so that in the unlikely event that your horse proves to be one of the few who are affected, you know what to look out for and what to do. Fortunately in this country we are not party to the growing trend that is occurring in the States of owners adminstering their own vaccines.
COPD - Chronic Obstrictive Pulmonary Disease
Perhaps still better known by some as broken wind or heaves, COPD is these days also termed RAO - Recurrent Airway Obstruction. Understandably a healthy respiratory system is vitally important for a horse but especially so if it is to undergo any form of exercise be it just hacking or competition. Whizzing about in the air are all sorts of nasties which can affect a horse's airways - viruses, bacteria, allergens, pollutants, etc - which, triggered by hypersensitivity, cause inflammation, and consequently therefore obstruction, of the respiratory passages.
Whilst it is thought that some horses may actually have an inherent predisposition to COPD, the most common causes are as a result of a physical reaction to fungal sporess contained in hay, bedding, etc. or as a consequence of a respiratory infection.
Experts think that a great many horses are affected to some degree or another but their owners are blissfully unaware that either anything is wrong at all, or do not realise it is COPD, so how do you know if your horse is suffering - what do you look out for?
a) reduced performance/ability to cope with the normal level of exercise
b)
laboured breathing during exercise or even at rest
c)
a persistent cough at rest exacerbated upon exercise
d)
a higher respiratory rate - 8/12 breaths/min is the average rate for a healthy horse whilst a COPD sufferers will increase to 20+
e)
a nasal discharge (usually white) from either or both nostrils
f)
a heave line may or may not be visible. but is in evidence in chronic cases as the muscles of the abdomen have to work that much harder to help the horse breathe.
Obviously if you suspect that your horse has any form of respiratory infection/disease you should seek the advice of your vet but here are some simple guidelines to help the COPD afflicted horse cope better or reduce the risk of your horse contracting it in the first place:
The stabled horse requires:
- plenty of ventilation but not a draft
-
dust-free bedding
-
clean, fresh water
-
good quality feedstuffs, both forage and concentrates. Consider switching to haylage, otherwise hay should be soaked (this causes fungal spores to swell so that they will be eaten rather than breathed in)
-
vaccination against infllluenza
ALSO:
DO NOT use a deep-litter bedding system (ammonia can act as an irritant).
DO NOT stable the horse next to others on straw.
DO NOT use a stable near to the muck heap pr hay/straw storage area.
Try to groom outside of the stable.
Remove horse from stable whilst mucking out.
Current research has established that horses affected by COPD etc. have lower levels of vitamin C in the lung Epithelial Lining Fluid than unaffected horses and that imbalances of oxidant to antioxidant may also be influential regarding general health of the lungs; vitamin c is an antioxidant. Tests have shown that the feeding of antioxidant products may help to maintain a healthy respiratory system and also help horses already suffering from COPD.
WOUND CLEANING
Proper cleaning of even the smallest of wounds is very important to ensure against bacterial infection. Whilst of course simple cuts do not normally cause any problems in themselves, if a horse has, for example, an unknown low white blood cell count then it will not have the neccessary defences to fight an infection; consequently a small nick can develop into something a bit more sinister.
The best way to ensure good hygiene is not to rub or even dab at the wound in the first instance but to trickle water from above it so that any bits of muck, grit, etc. are washed away rather than unconsciously pressed deeper into the wound cavity. Once this has been done over the wound and at its edges, then you can clean it properly.
Be careful in your use of antiseptic washes. Some can cause considerable drying of the skin immediately around the wound which can not only lead to skin tightness and hence discomfort, but the tighteness can actually sometimes impede healing as the wound is effectively being kept pulled open by the tautness; more importantly the drying effect some antiseptics have can also cause the skin to crack and in some cases these cracks can open up and become very sore and of course be further entry points for infection - something to be avoided at the best of times, but especially in mudfever cases.
HIBISCRUB is one of the best products for cleansing in our opinion but it is very powerful; used in too strong solution it can inhibit the growth of new tissue which, particularly in the case of wounds where there is a significant deficit of tissue (such as a tear types of wound) or those that need daily cleansing and dressing, can lead to a considerable slowing down of the production of new tissue.
There is the misconception that thus HIBISCRUB is a good product to use manage wounds that are exhibiting granulation tissue formation - but this is not the case - granulation tissue will form however much Hibiscrub has been used!
So when using HIBISCRUB remember that a weak solution is all that is required.
WARTS
Warts are quite common in young horses especially around their mouth and nose; in more severe cases the warts can spread further up the face. There may either be a collection of single warts, but more usually they are grouped very closely giving the typical “cauliflower floret” appearance. Although such warts are unsightly they do not pose any form of health threat and certainly do not affect the way a horse goes; they are just a cosmetic blemish.
Young horses are more usually prone to “wart attack” because their immune system is not firing on all cylinders – they have not yet acquired their full compliment of facial hair; this coupled with the much softer skin that the young horse has around his nose and mouth means that the pesky insects which carry the “wart virus”- papillomavirus – can more easily launch an attack.
Usually the warts will disappear - normally about 8/9 months from first appearing provided of course the horse is healthy and he lives in a well maintained environment (clean, etc.) - without any treatment being necessary as, as he matures, his defences improve and a natural immunity is built up. And as with so many similar viral infections, a secondary occurrence is not usual (although it can happen).
As warts are a viral infection they of course can be spread to other horses so good management practices need to be applied when dealing with an infected horse to try and limit their passing to other animals.
As with any infection though, there are instances where their presence gives a little more cause for concern – e.g. when the result of secondary infection. Secondary infection occurs when a wart gets damaged in some way and becomes reddened, sore and “open”; it is then prone to infection by other foreign bodies.
Many owners do opt to have the warts removed as by their very siting they can often interfere with the correct fitting of a noseband or can be chafed by bit rubbers, etc. thus increasing the risk of secondary infection and of course making the horse uncomfortable.
There are creams which remove warts very effectively available from your vet which are applied on, usually, a 3-day on/off cycle for 10-14 days. As the facial skin is so delicate the severe action of the cream does cause the skin to crack and become sore but once the warts have gone, there are plenty of ointments than can be applied to relieve such conditions.
Warts are self healing so the theory that surgical removal (which is really only feasible if numbers are low) bucks up the immune system and makes it start working more effectively against warts for itself is not proven.
If you notice warts appearing on other parts of your horse’s body i.e. other than on his muzzle and nose, then it could be an indication that his immune system is generally not working as it should be, in which case you should seek veterinary advice (there could be other reasons as well). If there is a malfunction with the immune system, then there will also be other signs that all is not well.
GRANULATION TISSUE
When a horse receives a wound part of the natural wound healing process in-built within the horse involves the production of what is known as “granulation tissue”; the process is a very important and necessary one.
So what exactly is granulation tissue
Granulation tissue is the correct terminology for what is commonly known as proud flesh.
This is the healing tissue that looks bobbly and bulgy when a wound starts to heal; it comprises tiny blood vessels and fibroplasts but contains no nerves. It develops on any wound anywhere on the body and is more commonly associated with wounds that have been left open rather than sutured (closed). Granulation tissue is important with regard to open wounds because it aids in infection resistance and then it gradually fills the open wound providing a surface for the new growth of epithelial (skin) cells to gradually form from the edges until the entire surface is covered with new, healthy skin. The photograph illustrates mild exuberant granulation tissue overgrowth which was readily removed with a scalpel and further growth inhibited by the application of a steriod lotion. |
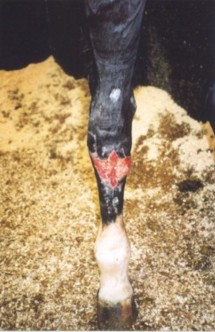 |
Despite granulation tissue formation being such a wonderful process, too much can sometimes be produced and this can cause problems. It sometimes grows so extensively and outwardly from a wound, looking like cabbage florets (hence the description "exhuberant granulation tissue") that it is necessary to take action to control it. Such formation is usually associated with wounds to the distal (lower) leg. If left, exuberant granulation tissue (e.g.t.) is not only unsightly but can stop a wound healing properly.
Several different factors are thought to stimulate the formation of excessive e.g.t. – the presence of very little soft tissue around the wound, infection, reduced blood supply and continual movement of the healing tissue – factors which explain why the lower limbs are mostly affected by severe proud flesh formation;these limbs do not have much extra skin and muscular padding (hence the stitching difficulties), this minimal skin also provides a restricted blood supply. Also lower limb wounds are more prone to infection from bedding, etc and obviously as the weight bearers are constantly “on the move”. Proud flesh forms very quickly indeed - wounds to joints being particularly vulnerable - and steps have to taken to prevent this.
Good wound management is paramount -scrupulous cleanliness is an absolute must. For lower limbs after initial dressing, wounds should be bandaged for a while, not only to assist in keeping the wound area clean but to restrict tissue movement around the wound itself; the pressure created by the bandage stops the naturally forming granulation tissue from becoming exuberant i.e. growing too vigorously.
Mild overgrowth of e.g.t. can be controlled by the application of a steriod ointment or lotion directly onto the tissue which restricts its production but if there is a considerable amount of e.g.t. then this is removed with a scalpel. The procedure is painless as there are no nerves in this type of tissue although it can be a bit gory because of the increased blood supply. In the cases of severe overgrowth removal has to be done either under anaesthetic or in several stages over a period of time because of the amount of blood loss.
Using a caustic agent to inhibit e.g.t. growth has to be done so with extreme caution and applied with great care as the newly forming healthy tissue can be severely damaged. As it is all too easy for such agents to be applied inappropriately or without due care, veterinary surgeons are reluctant to supply them for client application unless they can be sure of their competance to do so.
For wounds that are so large that there is a skin deficit, skin grafts are applied, but although this reduces the risk of infection and speeds healing, it does not eliminate the danger of e.g.t. formation.
Opinion is changing these days on how long to keep wounds covered, some advocating that the moist environment of a covered wound can actually slow down natural healing and encourage bacterial growth.
If you refer to Mia’s Story you will see that our vet was keen to leave dressings off the wound as soon as possible to allow air to it; o.k. so this put the onus on ourselves to maintain wound cleanliness but all the extra care needed and time taken has been well-worth it; we have been rewarded with a full sound horse with absolutely no proud flesh whatsoever.
BOTULISM
This is something most people do not hear much about and there are those that actually have never heard of it, but it is something everyone should be aware of.
With the advent of feeding haylage, there is a greater risk of horses being exposed to Botulism because of the very definite production methods that are required in order that this feedstuff is of a quality suitable for equines.
Haylage is not to be confused with silage; silage is extremely wet and is literally fermenting grasses, whilst haylage, although having a higher moisture content than hay, is considerably drier than silage. Haylage should smell very sweet, whereas silage smells somewhat unpleasant, and the more fermented it gets, the worse the odour! To produce good haylage for horses requires the wrapping process to be carried out at a very precise moment - when it is just moist enough to retain all its nutritional benefits, but dry enough so that it does not ferment (or rot) within the wrap - that's when botulism can take a ohold. The wrap must not be punctured prior to or during storage, air must not get in othewise the haylage will go mouldy.
Botulism is a micro-organism (clostridium botulism ) akin to tetanus but more deadly which thrives in anaerobic environments i.e. places where there is no oxygen; such places are rotting animal carcasses and compost heaps. If you open a bale of haylage and you have any concerns about its smell or colour or if you see any white (which is mould) or blackened (which is botulism) matter DO NOT FEED IT.